Within hours of arriving at Tree House Recovery, an all-male alcohol and drug treatment center in Costa Mesa, CA, Brian was clinging to a 12-foot inflatable river boat — in the way back, where they stick the new guys — and bracing himself for oncoming waves.
“Stroke!” demanded the coxswain as the boat began to drift, likely because Brian wasn’t paddling in sync with the other six recovering addicts on board. As a result, a series of intensifying waves hoisted the bow of the boat into the air, ejecting the 32-year-old lawyer from Ohio into the frigid, early morning surf. Frightened, barely sober and still adjusting to a wetsuit he’d initially put on backwards, Brian somehow remembered to place a hand on his head to indicate that he was okay. Before long, his fellow brothers in recovery scooped him from the Pacific Ocean, offering a round of hugs before returning him to his perch at the caboose.
Whatever that was, Brian thought, I want more of it.
That was the “Surf Passage,” part of Tree House Recovery’s “Action-Based Induction Therapy” that consists of team-based drills adapted from Navy SEAL training exercises. Just days earlier, Brian was incapacitated in a CVS parking lot with a fifth of vodka between his legs. “I was a big, big, big, big alcoholic,” he tells me. Before he got sober, everything in his life was dictated by booze, he explains. His withdrawals were so bad that when he woke up in the morning, he had to cling to the shower rail, lest he fall down. Four fingers of vodka were required to avoid throwing up so he could drive to work. Once there, Brian snuck shooters into plastic cups because he (mistakenly) thought vodka was odorless. Come nightfall, he’d drink another fifth or so. On weekends, he’d be blacked out by 11 a.m.
When he went to a doctor’s appointment for a routine checkup, they read his blood pressure at 215 over 135 and sent him to the ER. “Drinking’s going to kill you,” the EMT warned in the ambulance. A couple of days after completing a 30-day treatment program, though, Brian was thrust into a big trial, which he lost, once again bucking him from the wagon. His spiral was made worse by news that two of his four sisters were diagnosed with breast cancer.
On the sixth morning of the bender that followed, he bought a bottle of vodka at CVS and sat in his car awaiting the flight home to visit his ailing sisters. But when it came time to drive to the airport, he physically couldn’t operate the vehicle, which is when he says a light bulb went off. “I called American Addiction Centers and said, ‘I need help, and I need help like right now. Not two hours from now — this moment.’”
When a counselor arrived at the parking lot, Brian explained that he’d once managed to piece together 19 months of sobriety. She asked what he’d done during this time to relieve stress. “I’d just run a lot,” he replied. Based off that information, she recommended an exercise addiction treatment program at Tree House Recovery.
The National Council on Alcoholism and Drug Dependency estimates that more than 23 million Americans are addicted to alcohol and other drugs. To service these addicts, more than 4,000 treatment facilities are blanketed across the country, the vast majority of which are based either partially or entirely on the 12 Steps of Alcoholics Anonymous. The steps are so ingrained that many people — including medical professionals, academics and law enforcement — believe attending meetings and working with a sponsor to abstain from mind-altering substances is the only path to recovery.
But an increasing number of alternatives are basing their treatment plans on scientific research rather than adhering to a set of spiritual principles. SMART Recovery (Self-Management and Recovery Training), for example, is a cognitive behavioral therapy that focuses on the connection between thoughts, emotions and behaviors and encourages individuals not to admit powerlessness over addictions or use the concept of a “Higher Power.” Other 12-Step alternatives like Moderation Management and Rational Recovery preach harm reduction, a set of strategies intended to mitigate high-risk behaviors associated with substance abuse.
Then there’s the Tree House Surf Passage, in which seven guys on a raft must work and communicate cohesively to get beyond the surf before turning the boat around and riding a wave onto shore. It’s designed to reawaken the brain to the perception of being a social animal, explains Tree House founder and CEO Justin McMillen. “Some of the most powerful moments that we see in treatment happen on the beach with these guys,” he notes. “They’re realizing for the first time that they have this deep connection with somebody else, which ultimately equates to long-term connections that extend well after treatment.”
Like the Recovery Boot Camp in Florida, HisHouse in Northern California and ACE Recovery in South Carolina, Treehouse is exclusively for men. Reps from each of these centers offer me the same explanation as to why: Women are too bewildering for the addicted male brain. “The benefits of men-only rehab is there are no distractions,” explains Benji from HisHouse, a faith-based substance abuse program with four facilities in California. “Your mind is so messed up when you enter rehab, and it only gets more scattered if you’re thinking about women. What are you going to wear? What are you going to say? Why doesn’t the new girl like me? It’s just a shit fuck storm, man.”
As for gay patients: “We usually send them over to New Creation, our women’s house,” Benji says.
While McMillen, too, believes in a gendered approach to recovery, he’s quick to point out that Tree House also challenges traditional expectations of masculinity. “Our physical empowerment director is a Navy SEAL, but he sews as well. I have a background in ballet, but I can build a house, too. So we break stereotypes of what being a man is in a lot of ways.” He adds that one of the problems many of his clients have is an inability to find their own version of what being a man is. And so, at Tree House, they’re urged to become confident in themselves first and foremost — which could mean having the compassion of Gandhi or the gruffness of Columbo, so long as they’re able to take a joke.
Gender aside, McMillen was inspired by UCLA psychiatry professor Dan Siegel, who believes that our identity is shaped by relationships and that our brains are constantly being rewired based on these social connections. This philosophy formed the framework of the Tree House curriculum, designed to reawaken the brain into the perception of being a social animal. “We realized that by engaging in teamwork exercises, you engage and strengthen the brain,” McMillen says. “So we started layering different approaches onto that.”

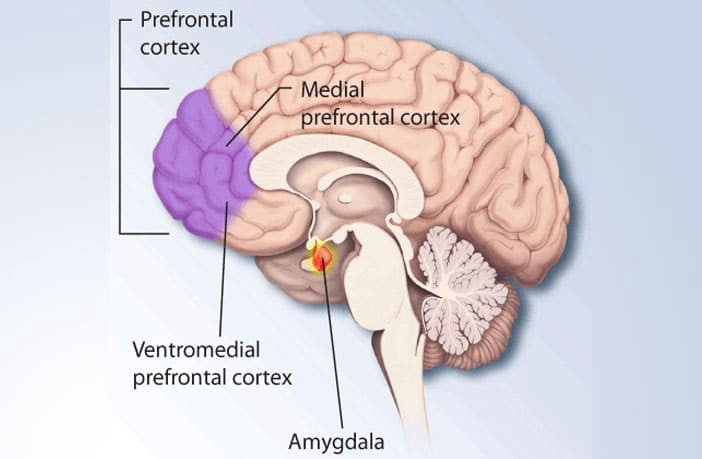
That’s why Action-Based Induction Therapy is just one of five modalities at Tree House. The others: Circuit training, yoga, writing therapy and addiction education. Put together, they’re meant to recondition the prefrontal cortex, essentially the brain’s quarterback. In particular, it’s responsible for nine critical functions — including empathy, impulse control, morality and human connection, all of which disappear in active addiction. When that happens, addicts — myself included — isolate, act recklessly and withdraw from society. This is what Tree House aims to reverse.
McMillen claims to be the only recovery center in the world doing such work. That said, different parts of it have a long history as therapeutic treatments. The Writing Therapy program, for example — designed to uncover and disempower past traumas — was created by George Coleman, a veteran intelligence specialist who returned from three combat tours with PTSD. A VA therapist introduced Coleman to the benefits of writing to shed light on traumatic incidents lurking in the dark, which inspired him to create Tree House’s Naked Writing curriculum. And many rehab facilities, like The Landing of Newport Beach, incorporate other cognitive behavioral therapies to help patients reframe negative and destructive thinking by re-engaging the prefrontal cortex.
To learn more about the relationship between the prefrontal cortex and addiction, I speak with Geoffrey Blaylock, the facility’s clinical director and writer of Tree House’s addiction education curriculum. Before anyone ever takes a drink or drug, Blaylock explains, adverse childhood experiences and traumas (e.g., death, violence, or physical/sexual abuse) can corrupt the brain’s normal development. Every single Tree House client has experienced some form of trauma, Blaylock says, which can include something as harmless as a childhood friend moving away. This corrupts the reward system of the brain — since trauma results in the brain producing fewer feel good neurotransmitters like dopamine — causing him to feel ostracized and/or abandoned, further inhibiting the functionality of the prefrontal cortex.
Basically then, the brains of Tree House clients are in a state of constant “fight or flight” mode. And when a stressed-out brain in constant survival mode — depressed because the reward system isn’t functioning correctly — comes in contact with substances for the first time, the stress hormones are mitigated, dopamine is suddenly firing and the limbic system (the “reptilian” part of the brain that governs the nervous system, reward and survival) falls in love. (I personally remember this moment vividly: Fourteen-years-old, staring in awe of an empty can of Budweiser I’d lifted from one of dad’s beer suitcases in the garage fridge.)
Afterwards, the reptilian brain begins urging — obsessively and compulsively — to continue ingesting drugs and alcohol as a number one priority — above eating, family and sex. And because the prefrontal cortex is compromised due to previous trauma, it’s unable to serve as the referee, allowing the limbic system to further overtake the brain. So when the addict is walking to the drug dealer, he or she isn’t in control. Rather, the part of the brain responsible for emotional reasoning — i.e., it’s probably not a good idea to steal from mom right now so I can get my fix — is essentially nonexistent.
To double-check Blaylock’s claims, I contact Dr. Michael Fox, an assistant professor of neurology at Harvard Medical School who specializes in the use of brain stimulation for the treatment of neurological diseases, including addiction. “Because the frontal lobe is one of the regions that’s a part of the addiction circuit, it makes sense to go after it as a possible therapeutic target,” he offers. “But exactly how you would intervene to help addiction remains scientifically unclear.”
Those interventions are clearer to Anto Bonci, scientific director at the National Institute on Drug Abuse. Bonci and his colleagues have found that chronic cocaine exposure in rats rendered the frontal region of the brain less active. “They were taking cocaine despite having some negative consequences related to food shortage,” he tells me. After finding this result in rats, Bonci used molecular technology called optogenetics to turn on their frontal regions. The result? Rats were no longer interested in the cocaine.
This led to a clinical trial using transcranial magnetic stimulation — a noninvasive way to stimulate the brain — to see whether stimulating the frontal regions of human cocaine addicts would likewise cause them to lose interest in the drug. “The majority of patients’ urine tested negative for cocaine, and their cocaine craving went down significantly,” Bonci explains. “Initial results from a larger, yet-to-be-published study on hundreds of patients are very similar: The majority of patients either significantly reduce their cocaine intake or quit completely.”
Bonci was unable to comment on Tree House specifically, but I asked, given that he’s found the prefrontal cortex to be undeniably associated with addiction, would it not make sense to focus on this area as a therapeutic target, as opposed to conceding that addicts are inherently powerless? “Absolutely,” he replies. “That’s exactly what we’re doing, and have initiated conversations with the FDA to seek approval for a new treatment against cocaine addiction.”
Catching waves would seem to beat the shit out of a lifetime of 12-Step meetings in church basements. And compared with AA, McMillen’s approach seems to be working. Granted, it’s a limited sample of 125, but 100 percent of clients treated in Tree House’s first year are currently sober five years out, as are 85 percent of all Tree House alumni to date. In contrast, a 2000 report in Alcoholism Treatment Quarterly found that, on average, 81 percent of newcomers stopped attending AA meetings within the first month. After 90 days, only 10 percent remained, a figure that was halved after a full year. Further, as Dr. Lance Dodes, a retired professor of psychiatry at Harvard Medical School, writes in The Sober Truth: Debunking the Bad Science Behind 12-Step Programs and the Rehab Industry, “Peer-reviewed studies peg the success rate of AA somewhere between five and 10 percent. About one of every 15 people who enter these programs is able to become and stay sober.”
And yet, since 1935, AA’s 12-Step Program of one alcoholic mentoring another has helped millions of people — again, myself included — recover from a seemingly hopeless condition. Two of my friends, Elvis and Bonnie, have each accrued 33 years of sobriety, which they credit to the program. “AA doesn’t work for everyone,” Bonnie admits. “But it’s worked for me for three decades. It’s free; it’s voluntary; and it’s readily available.”
“That’s probably what bothers the profiteers in the recovery business the most,” Elvis adds. (Recovery-business price points: Tree House is among the cheaper options at $13,500 a month — the program itself runs five months; meanwhile, inpatient rehab at Passages Malibu starts at $80,000 a month and Duffy’s Rehab in Napa Valley is $35,000 a month.)
While AA did help Brian remain sober for almost two years, he says working with one sponsor — as opposed to an entire staff of trained therapists also in recovery — ultimately proved to be ineffective for him. “AA is all about giving it up to God,” he explains. “If you have a great day, God made this happen for you. If you had a bad day, it’s okay because God will help you through it. There’s no accountability. Tree House is the opposite of that. If I have a great day, I own that victory because I created that, not because God did it for me. If I have a shitty day, I acknowledge I made mistakes and fell short. God’s not gonna pull me through that because it’s not God’s responsibility. It’s my responsibility.”
All steps aside, Brian credits Tree House’s success with its unwillingness to treat addiction with medication. “A lot of the other treatment centers out there are just trying to make addicts normal,” he adds. “Well, we’re not normal. And when you give us meds to make us normal, that only separates us from our authentic selves.”
Treating addiction with meds is what McMillen calls the “Medication Paradox.” On one hand, he says, you’re telling an addict to stop taking drugs to change the way they think and feel; on the other, you’re having them take prescription drugs to change the way they think and feel.

No comfort meds means the Tree House team must naturally exhaust clients throughout the day. So they’re up at 5 a.m. and in the water by 6 a.m., followed by 90 minutes in the gym, yoga, writing workshops and a series of one-on-one and group counseling sessions. Brian says the gym program — what Tree House calls “ESM,” the Latin abbreviation for Exercitium Semita Medela, or “Exercise as a Pathway to Healing” — was most beneficial for to him. A highly structured, fast-paced circuit and weight training hybrid — including cardio, interval training, core lifts, deadlifts, bench and squats — ESM utilizes proven methods of exercise coupled with motivational strategies. “When I went in, I couldn’t do a single push-up,” Brian says. “Not one. I had to do them from my knees.” Five months later, he can do more than 40.
More importantly, he explains, ESM returned his endorphins and serotonin levels to their necessary levels. “The only way our brains know how to release dopamine has been through the use of drugs and alcohol,” he says. “Now, suddenly, those have been removed. It takes some time, but what you realize is that through physical exercise, you don’t need any of that. Your body will heal itself if you put it in the right environment and you treat it the right way. For the first time in my life without drugs or alcohol, I can sleep. My anxiety is pretty much nonexistent. I look like an athlete. I’m not an athlete. But I look like one.“
Another central focus at the Tree House, which also borrows from PTSD therapy, is reintroducing platonic touch. I’m hugged no less than a dozen times over the two days I spend there. And not just a pat on the back — these are long, meaningful hugs, often accompanied by a gentle sway. “In the military, we were taught that if you’re cold, cuddle up against the next guy,” says Neil Trusso, the aforementioned former Navy SEAL and the Tree House’s physical empowerment director. More importantly, McMillen adds, active addiction is one of the loneliest states of humanity, while touch increases feel-good hormones and raises oxytocin, a bonding chemical that enhances trust. One way Tree House encourages platonic touch during Action-Based Induction Therapy is to have clients sit with their backs to the waves and link their arms. “Boundaries magically fade away,” McMillen says, “because it’s more about staying warm and holding on to prevent being swept away by the surf.”
Tree House is moving up the coast, too. Last year, it opened a second location in Portland, Oregon, McMillen’s hometown. And over the next five years, there are plans to open 32 centers nationwide — from Hawaii to Tennessee to Kansas to Montana (and all stops in between). Also in 2017, Tree House was invited to provide insight on how to fight the opioid epidemic by participating in a study session in Washington, D.C., related to the Comprehensive Addiction and Recovery Act, signed into law by President Obama in 2016. “We focused on establishing standards for assessing health outcomes during and after care as well as the implementation of a pay-for-performance reimbursement model for insurance companies, which align financial incentives with better outcomes rather than the current system of rewarding volume and intensity of care delivered,” says McMillen. “We feel strongly that if our industry was forced to innovate and get better in order to get paid, a lot more people would recover from addiction.”
As for Brian, he’s excited to graduate from Tree House in the next couple of weeks, but he says he’s in no hurry to leave. In fact, he plans to stay in Costa Mesa after graduation and transition into a sober-living house. “I cannot go back to living in an apartment by myself and isolating,” he explains. “I stop moving. I stop exercising. I stop meditating. It’s a slow progression, but over time, you lose everything.”

