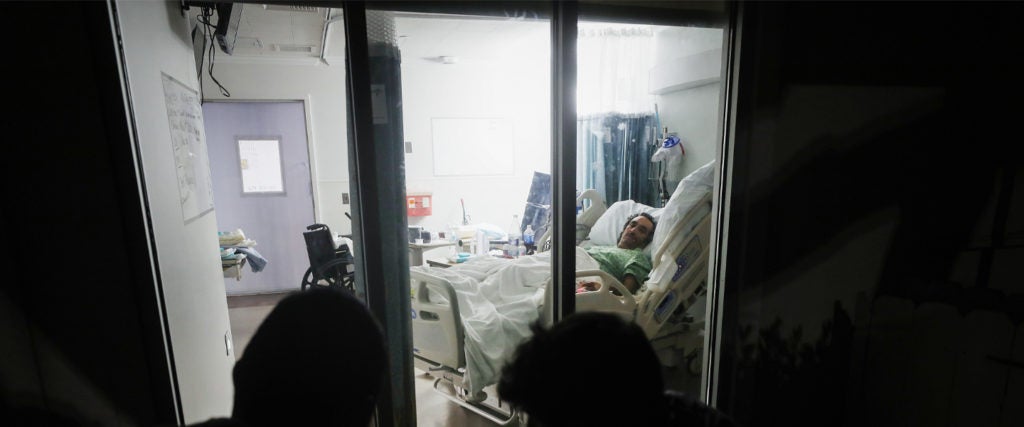
I thought my pandemic experience was lonely until I met Jim, a 54-year-old photographer/producer who contracted coronavirus at the end of March, likely from his wife who works at the University of Oregon in Eugene, which is where they live together. Although they were lucky enough to avoid hospitalization, they were both too weak to walk to their mailbox for weeks and sick for well over a month. “It was like the worst flu you ever had, times 10,” Jim recalls.
Friends, family and neighbors have been helpful with checking in on them and making grocery runs during their quarantine, but they’ve otherwise avoided him “like the plague,” he says.
Now about six and a half weeks since their symptoms have resolved — and even as their state opens up — “no one wants to come over to visit nor have we received any invitations,” he tells me. “We dropped off a bottle of wine to the friends who had brought us groceries while we were sick, and we were asked to leave it at the front door.”
In this regard at least, Jim isn’t alone. The more scientists uncover about how the virus sheds and spreads, the less reassurance people with confirmed infections have about ever being able to socialize again. As of now, experts suspect individuals who contract coronavirus are most contagious during the pre-symptomatic stage — i.e., the first few days before they start to feel sick. They then remain contagious for about another 10 days after that (which is where the recommended 14-day quarantine originates from).
However, as the virus continues to attack people in new and confounding ways, leaving patients like Jim debilitatingly ill far beyond the two-week mark, it’s only raised more questions about how long people can pass on the virus. Anne Liu, an infectious disease physician at Stanford University, confirms that no one knows enough about COVID-19 to be sure how long people are contagious for. “It probably varies a lot, and it may vary by severity, but that’s all to be determined,” she explains. “We don’t know if resolution of symptoms means that a person is no longer contagious.”
There are two main types of COVID-19 tests currently available: 1) the polymerise chain reaction test (nasal swabs looking for active infections); and 2) serologic or antibody tests (blood samples used to track past infections). By now, most of us know that COVID-19 PCR tests have about a 20 percent false-negative rate, but that’s only part of the problem when trying to pin down how long people are contagious for.
According to Liu, the majority of the data doctors are currently working with is from PCR tests, which demonstrate the presence of viral RNA but doesn’t show whether the virus is dead or alive. Scientists suspect PCR tests may remain positive beyond the contagiousness period, because the virus remains active for about a week after the onset of symptoms. They’re not sure, though, that an inactive virus means a person is safe to be social again. “Whether this correlates to being contagious is unknown,” she warns.
Even less is known about what antibody tests actually mean, but Liu and other experts believe at best, antibodies only offer protection for about two to three months. Not to mention, not everyone who contracts COVID-19 will necessarily test positive for antibodies. This could be because they took an antibody test too early and should’ve taken a PCR test first, or that they should have taken it in conjunction with the antibody test.
“The PCR is positive and antibodies are negative early in disease,” Liu explains. “The other part of the answer is that some patients who recover from COVID can have negative antibodies, but they’re probably in the minority. It may also happen more in patients who never developed symptoms. It isn’t yet known why this happens.”
For many people who claim to have “probably already had COVID,” the science shatters that sense of security. Even if you contracted it back in February or March, you’re not necessarily protected from getting it again or passing it on to someone else. “The number of people I’ve had tell me they think they’ve had it is wild,” says Molly, a 27-year-old account executive in New York City. “People are just expecting there’s immunity, and there’s no proof of that.”
She would know. Despite being young and otherwise healthy, she got very sick for 12 days in early March. “I was lucky I was never on a ventilator or anything, but my body pains were really bad,” she tells me. But since she was an early victim of the pandemic, she found herself being pretty popular among her friend group once she started feeling like herself again. Most of them thought she was safe to hang around because she already had it. To her credit, however, she still held off on seeing people until NYC started opening back up again earlier this month — and even then, only outdoors, with masks, while maintaining social distancing. “I was afraid to go near people for a while because I felt like I could hurt them,” she says.
To Liu, the takeaways are simple: Everyone should operate as if they can contract the coronavirus and pass it on at any point, regardless of whether they’ve been sick previously or tested positive for antibodies. “The criteria for restarting social interactions varies a lot and will continue to change as we learn about the virus,” Liu says. “In the meantime, people who have recovered from infection should continue wearing a mask, at the very least, and distancing when possible.”
To that end, Jim and his wife have kept their socializing to Zoom hangouts and waving to neighbors out the windows. And as much as he misses his pre-pandemic life, Jim doesn’t blame anyone for keeping their distance. “I wouldn’t wish Coronavirus on my worst enemy,” he tells me. “It was miserable and terrifying.”